Medical school and pregnancy: can you really have it all?
1 College of Osteopathic Medicine of the Pacific-Northwest, Western University of Health Sciences, Lebanon, OR
2 Providence St. Peter Family Medicine, Olympia, WA
3 Oregon Health & Sciences University Hillsboro Medical Center, Hillsboro, OR
4 Madigan Army Medical Center, Tacoma, WA
5 University of Tennessee Graduate School of Medicine, Knoxville, TN
6 Spokane Teaching Health Center, Spokane, WA
ES: https://orcid.org/0000-0002-6999-079X
LB: https://orcid.org/0000-0002-3380-0624
KV: https://orcid.org/0009-0006-8277-9450
TD: https://orcid.org/0009-0004-1378-6142
PL: https://orcid.org/0009-0003-4581-6740
ES: https://orcid.org/0009-0005-4609-6102
Abstract
Background
Since 2017 the majority of U.S. medical students have been female, and many face the decision of starting a family during the rigors of medical training or waiting an average of almost 10 years to finish residency.
Methods
This study solicited medical students’ views and opinions on being pregnant during medical school. A survey on pregnancy during medical school was sent to 38 U.S. osteopathic medical schools, and 13 agreed to distribute it to their student population. In total, 64 responses were eligible and analyzed.
Results
Of 64 complete responses, 49 (76.6%) had previously been pregnant during medical school and 15 (23.4%) were currently pregnant. The average age of first pregnancy was 26.6 years (SD = 3.2). 83.9% (n = 52) of respondents felt pregnancy affected their medical studies. Attending medical school in the Southern U.S. was significantly associated with less perceived support from faculty and less support transitioning back to curriculum after pregnancy. Student comments revealed negative experiences around curricular flexibility and ability to take time off.
Conclusions
Pregnancy is a unique experience for medical students, and often entails decisions and sacrifices which medical students may feel they face without the support of their school. With little flexibility, medical schools’ support structures and policies regarding pregnancy may be outdated and inadequate for many students.
Keywords: medical education, medical students, pregnancy
Introduction
The experiences of students who become pregnant during medical school are under-researched, especially given that the majority of U.S. medical students have identified as female since 2017 [1]. Medical students who want children face pregnancy, delivery, and post-partum during the rigors of medical school, or wait between seven and fourteen years to finish training [2]. Medical students’ average age at matriculation is 22 (allopathic) and 25 (osteopathic), so waiting puts students in a difficult position as they plan their future, possibly exposing them to risks associated with a geriatric pregnancy, particularly if they plan for more than one child [3,4]. There is evidence to suggest that nearly 75% of female physicians delay childbearing, resulting in a growing number confronting infertility [5]. Conversely, choosing to become pregnant during medical training comes with its own risks, including deciding whether to take time off and how much, the possibility of complications which delay family planning or require unplanned time off, loss of future earnings, and additional financial costs [6,7].
Currently, approximately one-third of medical schools have a parental leave policy at all, and those may not be comprehensive or adequate [8,9]. Few schools allow for the twelve weeks of leave recommended by the Policy Center for Maternal Mental Health without the student becoming unable to graduate on time, and many have no dispensation for partner leave (if the partner is in medical school) or leave for adoption or fostering [8].
Methods and Materials
This study is a mixed-methods, observational, survey-based design. It was approved by the Institutional Review Board of Western University of Health Sciences (#1636473) prior to data collection. All students gave their written consent for the use of their anonymous data to be used in research.
Setting
The national survey was administered via Qualtrics and was open from July to September 2022.
Sampling and participants
Osteopathic medical students were chosen specifically for this study because they have a higher mean age and therefore may be more affected by decisions around parenthood. Participation requests were sent to 38 of the 41 accredited osteopathic medical schools in the U.S. at the time; contact could not be made in three cases. Approval was issued by thirteen schools, who each disseminated the survey to all classes of their medical student body through university email, a total distribution n = ~9,300. Inclusion criteria included being 18 or older, a current osteopathic medical student of any year in school, and currently or previously pregnant during any portion of medical school.
Measurement tools
This study was guided by the National Academy of Medicine (NAM) Model, a conceptual framework which describes factors impacting clinician well-being [10]. NAM Model factors adopted were (1) socio-cultural; (2) learning/practice environment; and (3) personal [10]. A 20-question survey was developed to assess these factors and was tested in a focus group for understandability and completeness, and changes were made based on their feedback. See Appendix 1 for the survey.
Data collection
Qualtrics and Excel were used for data collection. No compensation was offered for participation. All survey responses were anonymous, and school names were collapsed into regions for analysis.
Data analysis
Quantitative: Raw data was cleaned, coded, and uploaded into SPSS (v. 28) for analysis. Assumptions of data normality and homogeneity of variance were checked, and data met criteria for the ensuing statistical tests. Descriptive statistics were done to examine student characteristics, and ANOVAs with Dunnett’s T2 post-hoc analysis were performed to determine if there were significant differences by region, year in school, or age of first pregnancy. The alpha level was set at 0.05.
Qualitative: The goal of collecting qualitative data was to obtain student experiences in their own words [11]. This was accomplished with text boxes throughout the survey. Six phases of qualitative assessment were undertaken, and completed by a researcher experienced in qualitative coding, including two passes of the data identifying interesting concepts (codes), generating a list of potential themes from the codes, combining and analyzing potential themes for similarities and relevance, matching themes with specific quotes, and analyzing themes by tying them back to the research questions [11].
Psychometric Analysis: Cronbach’s 𝞪 was used to assess the internal consistency (reliability) of the scale as a whole. Pearson’s correlation coefficient matrix was compared with Pearson’s critical values to assess validity.
Results
Student characteristics
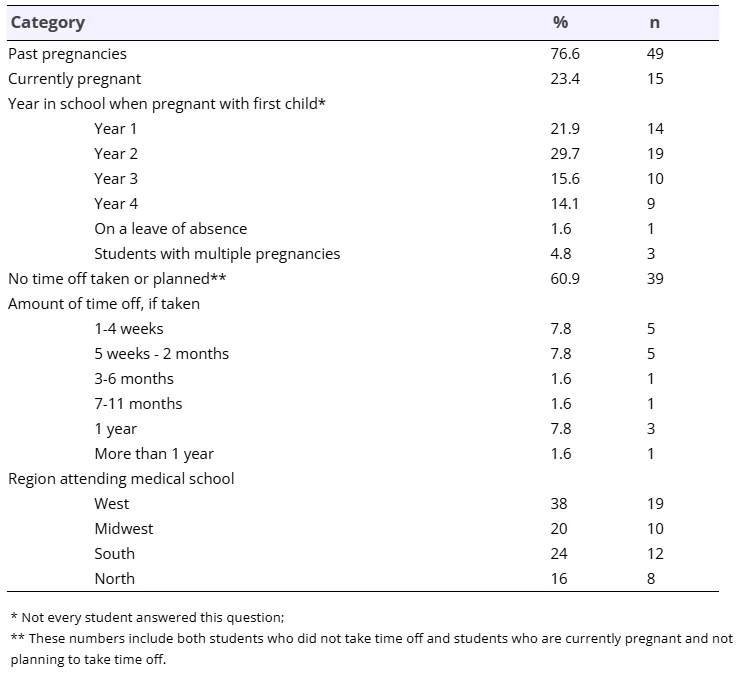
Out of ~9,300 surveys sent, a total of 189 responses were received, a response rate of 2%. Of those responses, 70 reported previous or current pregnancy during medical school. Six of these responses were missing all data and so were excluded, leaving a final overall n = 64. Of the students who listed a school name, n = 19 (38%) were attending school in the West, n = 12 (24%) in the South, n = 10 (20%) in the Midwest, and n = 8 (16%) in the Northeast [12]. See Table 1 for student characteristics.
The majority of students were in preclinical years during pregnancy (n = 33, 54.7%). The average time during schooling that students became pregnant was towards the end of their second year (M = 2.83, SD = 2.01), and the mean age of pregnancy was 26.6 years (SD = 3.2) with a range of 21 – 41 years.
Decisions regarding time off
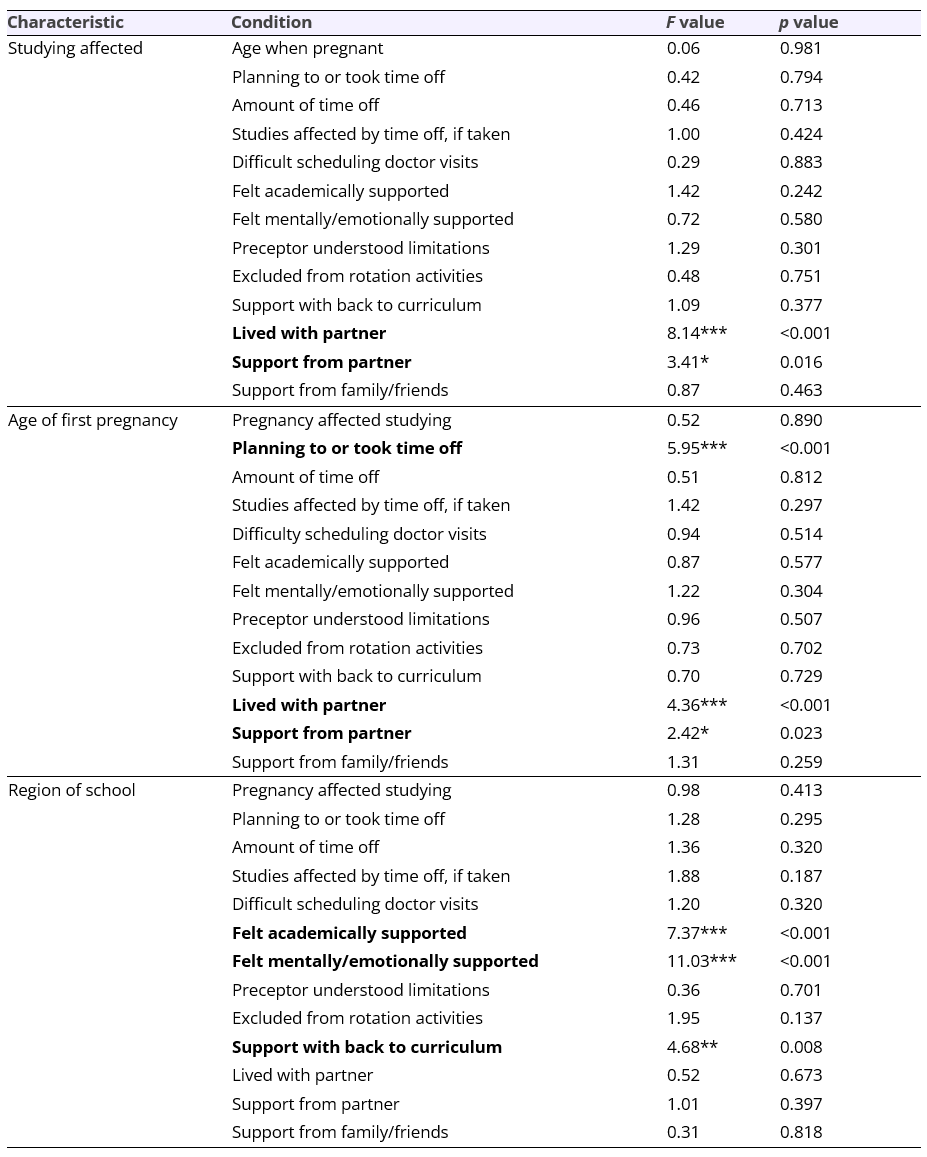
Most students (n = 39, 60.9%) reported not taking or not planning to take any time off during/after pregnancy. Of those who had or were planning to take time off, the most frequent choices were 5-8 weeks or one year. Only one student each reported taking off two weeks or less, 3-6 months, 7-11 months, or more than one year. Of those who took time off, most said the time off very or somewhat negatively affected their studies (n = 18, 55.6%). The age that someone became pregnant in medical school was significantly associated with taking time off, such that the older a student was, the higher the likelihood they would take time off (F(12,43) = 5.96, p < 0.001). We focused on first pregnancies as we expected that most pregnant students would be managing their first pregnancy given the average age of medical students, and assessed age at first pregnancy in order to assess if medical students were waiting to become pregnant. See Table 2 for ANOVA results.
Students who attended a school with an explicitly stated pregnancy leave policy, two of the thirteen schools, reported taking significantly more time off or planning to take significantly more time off (t = 4.93, p < 0.001), though were not significantly more likely to report feeling better supported by faculty or their institution. Overall, students reported difficulty navigating time off. One said, “I feel like I wasn't offered options for what I could do for time off or moving required events around.” Another student summarized the issue of little time off versus what she thought was excessive time off: “I was told I could use my 3 weeks of flex time/vacation [in my] 4th year and then a 2-week online rotation. […] Otherwise I would have to take a year-long leave of absence.” Another student reported a similar experience: “When I mentioned I was pregnant, [I] was ‘kindly’ offered to take a leave of absence for a year rather than working together to find a good way to continue rotations/school.” Finally: “The school was only willing to give me 2 weeks off and my husband [also a medical student] only 2 days.”
Several students reported a more positive experience, often related to their own efforts to time their pregnancies as best they could: “My baby was born the first day of my Christmas break during my second year, so I was able to have a whole month at home while also not taking any time off from school.” “My experience during pregnancy was positive since I was doing a fellowship year between 2nd and 3rd year. I can almost guarantee that I would not feel this way if the timing were not to work this way.” In addition, students mentioned that the change to virtual curriculum that medical schools made with the onset of the COVID-19 pandemic was beneficial: “I was pregnant during the pandemic […] when most of [the] curriculum was held virtually. This gave me a lot more flexibility to schedule appointments…” [13].
Support from faculty
Some students (n = 18, 26.5%) reported feeling strongly academically supported by faculty, though most reported moderate support (n = 21, 30.9%), and several (n = 11, 16.2%) did not feel supported at all. Findings were similar for students feeling emotionally or mentally supported by faculty (strongly: n = 17, 28.3%; somewhat: n = 20, 33.3%; not supported: n = 14, 23.3%). Student comments included: “There is not a lot of understanding from course instructors and with scheduling. You may be ‘excused’ from some activities due to doctors’ appointments or child related things but […] you aren’t given any additional time/considerations.” One student had a particularly negative experience: “I explained my pregnancy-related symptoms/conditions such as HG [hyperemesis gravidarum, a condition of severe nausea and vomiting during pregnancy [14] and I was not met with sympathy nor compassion. Instead I was constantly pressured to keep attendance and scores up.”
Institutional support
One quarter of students (n = 13, 25%) reported no support whatsoever from their programs in transitioning back to curriculum, regardless of time off. Though most noted moderate (n = 19, 36.6%) or a great deal of support (n = 10, 19.2%), comments were generally negative: “I had to sit for a 3-hour exam 5 days after vaginal delivery. I was not granted more time or breaks.” Another student reported: “I experienced a molar pregnancy while studying for level 1 in summer of 2021 after 2nd year […] and the school was very unsupportive […] I took a COMSAE [a 200-question exam] on the bathroom floor while actively vomiting because it had to be done by that day.” Students who pursued further resources also met with barriers: “The resource and accommodations center said pregnancy was not a disability and thus could not support me. […] Not having a standard protocol left room for the deans’ personal views which heavily influenced […] my lack of support.” Another student stated: “[I was] made to feel like I was being punished for starting my family. Still dealing with the ramifications 2 years later.”
Preceptor relationships and perceived exclusion from clinical learning opportunities
Of the students who were on rotations during their pregnancies, all reported that their preceptors were very or somewhat understanding (n = 21, 38.9%). Comments focused on the contrast between preceptor support versus institutional support: “[…] my rotation site was supportive but my school did not feel supportive.” A second student noted: “I had a very difficult pregnancy and felt like I had very little support/understanding from my program. There were some individuals (preceptors mostly) that were very understanding and worked with me, for which I was very thankful.”
Most students reported no perception of exclusion from learning opportunities when on rotations while pregnant (n = 43, 84.3%). However, osteopathic medical students do many hours of osteopathic manipulative medicine (OMM), for which there are pregnancy precautions [15]. Student comments reflect this: “[I could not] perform or have OMT treatments.” “I could not perform the […] treatment due to the necessity of using my abdomen.” Another student reported barriers to anatomy curriculum which resulted in her not receiving required curriculum: “I was not allowed in anatomy lab during the first trimester and was not given an online course to supplement the material.”
Perceptions of scheduling prenatal visits
The majority of students (n = 28, 51.8%) reported it was extremely or somewhat difficult to schedule prenatal visits. Student comments included, “Sometimes it was difficult to manage harder rotations/hours and scheduling doctor’s appointments […] I worked really hard to optimize my schedule for that year…” Again, students cited the curricular changes related to the COVID-19 pandemic as assisting them in time-management: “COVID really affected my experience with pregnancy during medical school because we were virtual. This made it easier to schedule appointments and keep up with school[…].”
Regional differences
Statistically significant differences were found between regions of the U.S. for perceptions of academic support from faculty (F(3,45) = 7.37, p < 0.001), mental/emotional support from faculty (F(3,45) = 11.03, p < 0.001), and support transitioning back into curriculum after giving birth (F(3,33) = 4.68, p = 0.008). Dunnett T3 post-hoc analysis revealed that regions differed on feeling academically supported (MD West vs. South = -0.71, p = 0.002; MD Midwest vs. South = -1.29, p < 0.001; Northeast vs. South not significant); emotionally/mentally supported (MD West vs. South = -0.71, p = 0.003; MD Midwest vs. South = -1.59, p < 0.001; MD Northeast vs. South = -1.14, p = 0.11), and supported in transitioning back into curriculum after delivery (MD West vs. South = -1.69, p = 0.020; MD Midwest vs. South = -2.30, p = 0.005; Northeast vs. South not significant) [12].
Perceived effects on ability to study
The majority of students (n = 52, 83.9%) said pregnancy definitely or probably affected their studying negatively. However, one student noted, “Being pregnant while in medical school actually taught me how to study more effectively […] I learned how to achieve similar grades with less time […].”
Social support
The majority of students reported they lived with a partner during their pregnancy (n = 52, 81.3%), and most reported receiving a lot or a moderate amount of support from partners (n = 45, 93.7%) and family and friends (n = 43, 86%). Having a live-in partner had a significantly beneficial effect on studying during pregnancy (F(4,50) = 8.14, p < 0.001), with the more perceived support from a partner associated with better studying (F(4,46) = 3.41, p = 0.016).
Student comments noted the value of having a partner: “My husband also became a stay-at-home dad, if not, it wouldn’t have been possible for me to not take time off.” In one case, a student cited the lack of social support which led her to make an important decision: “I decided to have an abortion in fear of not being supported by my family and not being able to financially support my child while on loans […].”
Psychometric analysis
Cronbach’s 𝞪 was calculated to assess internal consistency reliability, and was 0.57, a moderate level, for Likert scale items. Validity was assessed by comparing Pearson’s correlation coefficient matrix of total scores to Pearson’s critical value (r = 0.20), and evidence of validity was found for all Likert scale items. Future studies considering use of the survey would benefit from further psychometric refinement prior to use.
Discussion
This study explored the pregnancy experiences of n = 64 osteopathic medical students. Key results included a majority of students not taking any time off, sometimes even when experiencing severe symptoms. There were generally positive perceptions of preceptor relationships and negative perceptions around institutional policies and support, even though greater than 50% of students reported positive institutional support. This may have been due to qualitative comments being disproportionately from students who had negative experiences.
Decisions around time off were likely related to institutional support or lack thereof, particularly as students at schools with explicit policies on pregnancy leave took or were planning to take significantly more time off. The finding that time off, if taken, was split between 5-8 weeks and one year suggests that if students chose or needed to take time off, they either minimized it to remain on track with graduation or they took a year off, with few options in between. Taking an entire year off may be quite impactful, particularly when student loan support and health insurance terminate after a few months.[16] Individuals who take maternity leave also have reduced lifetime earnings, and those with higher wages, such as physicians, have an even more significant loss of lifetime earnings [17]. While a full discussion on parental leave policy in the U.S. is beyond the scope of this paper, research supports that parental leave has extensive, positive impacts on the mental and physical health of parents and children [18].
Patterns were noted regionally, although sample sizes were small. The level of perceived support academically, mentally/emotionally, and for return to curriculum were all higher among students attending schools in the West and Midwest [12]. Students in the South reported feeling more excluded from clinical learning opportunities than students in the West. Mandatory versus voluntary paid maternity leave, who regulates it, and the amount given may explain regional differences [19].
Policies around COVID-19 also varied by region. Numerous qualitative comments emphasized the role of COVID-19 in requiring programs to deploy asynchronous learning modalities, which by nature are more flexible. Students conveyed that the COVID-19 pandemic gave them flexibility during medical school to effectively balance the priorities of curriculum and prenatal appointments. A recent study showed that 142 of the 149 allopathic and osteopathic medical schools in the U.S. implemented at least partially virtual pre-clinical curriculum in 2020-2021, and 64 retained at least some of this flexibility for the 2021-2022 academic year [20]. Older students also reported taking more time off, which may have been related to more flexibility during the clinical years, or perhaps already having children at home to care for.
Limitations and future directions
This study has several important limitations. Selection bias is likely present, as those who felt passionate about their difficult experiences may be more apt to participate. Additionally, this study may have recall bias as it required some students to recall their previous experiences of pregnancy. Despite reaching out to all osteopathic medical schools throughout the country, only 64 eligible responses were received, thus limiting the sample size in terms of raw numbers as well as demographics and geographical distribution. A larger sample size would be needed before results would be generalizable. This study did not explore whether the pregnancies in question were planned, but with nearly half of pregnancies in the U.S. unplanned, this is a worthwhile consideration for future research [21]. Racial and ethnic diversity and gender are important factors to understand the true experiences of pregnancy in medical school, and important to study in the future due to the additional stressors that students with marginalized identities face [22-24]. We left these factors out of this study to minimize response burden.
Future studies regarding miscarriages and/or abortions during medical school; the experiences of partners of pregnant people; pregnancy in people who do not identify as female; people who enter medical school as parents; differences between returning to preclinical years which have a regular daytime schedule versus returning to clinical rotations which may be overnight or long hours; MD versus DO school pregnancy policies; and postpartum challenges such as breastfeeding, finding adequate and affordable childcare, and maintaining financial stability would also be beneficial to understanding the medical school experience. For example, finding time and private space for pumping breastmilk may be difficult in a clinical setting, as evidenced by the American Academy of Family Physicians’ statement that lactating physicians can wear a breast pump in the operating room so their work is not interrupted [25]. The American Academy of Family Physicians, American College of Obstetricians and Gynecologists, and the American Academy of Pediatrics recommend a minimum of twelve, eight, and six weeks paid parental leave, respectively [26-29]. As noted, medical students may be forced to choose between leave that is significantly shorter or longer than this.
In our view, considerations for improvement include having a parental leave policy which includes additional flexibility around time off, periods of virtual coursework, more reasonable timelines for making up work, and extending financial aid and health insurance while on leave. Given the curricular flexibility that medical schools implemented during the COVID-19 pandemic, allowing a period of virtual curriculum instead of having to take time off completely, or permitting a virtual transition period back to curriculum, could potentially be feasible [13]. Students may also wish to consider the region when choosing a medical school.
Ultimately, potential medical school candidates may rank medical schools by support for major life events like pregnancy. The issue is likely to become more urgent as burnout rates increase each year in students and healthcare professionals, particularly as females in medicine show higher rates of personal distress and emotional exhaustion [30,31]. We think family planning during medical training needs a long overdue adjustment to allow medical students to start a family when it’s best for them, without being penalized by their schools or sacrificing future income.
Acknowledgments
None.
Author Contributions
Edie Sperling: Supervision, methodology, formal analysis, writing the original draft
Lillie Blair: Conceptualization, investigation, review and editing
Kiran Varani: Conceptualization, investigation, writing the original draft
Taylor Deyoe: Conceptualization, investigation, review and editing
Paige Lay: Conceptualization, investigation, review and editing
Emily Swanson: Conceptualization, investigation, review and editing
Data Availability
Data for this study can be found at the persistent link: https://www.kaggle.com/datasets/esperling/pregnancy-in-osteopathic-medical-school-survey
Transparent Peer Review
Results from the Transparent Peer Review can be found here.
Recommended Citation
Sperling, E., Blair, L., Varani, K., Deyoe, T., Lay, P., & Swanson, E. (2025). Medical school and pregnancy: can you really have it all? Stacks Journal: 25010. https://doi.org/10.60102/stacks-25010
References
- Murphy B. Women in medical schools: Dig into the latest record-breaking numbers. AMA. 2021 Sept 29. Available at: https://www.ama-assn.org/education/medical-school-diversity/women-medical-schools-dig-latest-record-breaking-numbers#:~:text=Protecting%20your%20future%20as%20a,the%20number%20of%20students%20matriculating.
- Length of Residencies. Career Counseling Office Residency Roadmap. Washington University School of Medicine in St. Louis. Available at: https://residency.wustl.edu/residencies/length-of-residencies/
- Sees JP, Nahian A, Johnson R. A 10-year report on the trends of osteopathic medical students (OMS) in osteopathic orthopaedic residency over the past decade. 2023; 7(1):1-10.
- Correa-de-Araujo R, Yoon SS. Clinical outcomes in high-risk pregnancies due to advanced maternal age. Journal of Women’s Health. 2021 Feb;30(2):160–7.
- Bakkensen JB, Smith KS, Cheung EO, Moreno PI, Goldman KN, Lawson AK, et al. Childbearing, infertility, and career trajectories among women in medicine. JAMA Network Open. 2023 Jul 27;6(7):e2326192.
- Liebhardt H, Stolz K, Mörtl K, Prospero K, Niehues J, Fegert J. Starting a family during medical studies? Results of a pilot study on family friendliness in the study of medicine at the University of Ulm. GMS Z Med Ausbild. 2011;28(1):Doc14. doi: 10.3205/zma000726.
- Cujec B, Oancia T, Bohm C, Johnson D. Career and parenting satisfaction among medical students, residents and physician teachers at a Canadian medical school. CMAJ. 2000 Mar 7;162(5):637-40. PMID: 10738448; PMCID: PMC1231217.
- Kraus M, Talbott J, Melikian R, Merrill S, Stonnington, Hayes S, et al. Current parental leave policies for medical students at U.S. medical schools: A comparative study. Academic medicine : Journal of the Association of American Medical Colleges.. 2021;96(9). Available from: https://pubmed.ncbi.nlm.nih.gov/33769337/
- Roselin D, Lee J, Jagsi R, Blair-Loy M, Ira K, Dahiya P, et al. Medical student parental leave policies at U.S. medical schools. J Womens Health (Larchmt). 2022 Oct;31(10):1403–10
- Brigham T, Barden C, Legreid Dopp A, Hengerer A, Kaplan J, Malone B, et al. A journey to construct an all-encompassing conceptual model of factors affecting clinician well-being and resilience. NAM Perspectives. 2021. 96:1315-1318.
- Merriam SB, Tisdell EJ. Qualitative Research in Practice: Examples for Discussion and Analysis. San Francisco, CA: Jossey-Bass; 2002.
- Geographic region. Health, United States, 2020-2021. Centers for Disease Control and Prevention. Available at: https://www.cdc.gov/nchs/hus/sources-definitions/geographic-region.htm
- Kempthorne D, Williams L, Brazelle M, Obi T, Shao C, Kennedy G, et al. Navigating the virtual medical school experience during COVID – What comes next? Amer JSurg. 2022 May;223(5):1013.
- Jennings LK, Mahdy H. Hyperemesis Gravidarum. StatPearls. 2023; Available from: http://www.ncbi.nlm.nih.gov/books/NBK532917/
- Stickler K, Kearns G. Spinal manipulation and adverse event reporting in the pregnant patient limits estimation of relative risk: A narrative review. JMMT. 2023 May 4;31(3):162–73.
- Taking a break from your medical education. American Association of Medical Colleges. 2023, Dec 26. Available at: https://students-residents.aamc.org/financial-aid-resources/taking-break-your-medical-education
- Dechter EK. Maternity leave, effort allocation, and postmotherhood earnings. HCJ. 2014 Jun;8(2):97–125.
- Van Niel MS, Bhatia R, Riano NS, de Faria L, Catapano-Friedman L, Ravven S, et al. The impact of paid maternity leave on the mental and physical health of mothers and children: A review of the literature and policy implications. Harv Rev Psychiatry. 2020 Apr;28(2):113.
- State paid family leave laws across the U.S. Bipartisan Policy Center. 2024, Jan 16. Available at: https://bipartisanpolicy.org/explainer/state-paid-family-leave-laws-across-the-u-s/
- Curricular reports. American Association of Medical Colleges. 2022. Available at: https://www.aamc.org/data-reports/curriculum-reports/data/covid-19-pandemic-changes-curriculum
- Prevent unintended pregnancy. Centers for Disease Control and Prevention. 2022, March 10. Available at: https://archive.cdc.gov/#/details?q=prevent%20unintended%20pregnancy&start=0&rows=10&url=https://www.cdc.gov/sixeighteen/pregnancy/index.htm
- Berger M, Sarnyai Z. “More than skin deep”: stress neurobiology and mental health consequences of racial discrimination. Stress. 2015 Jan 2;18(1):1–10.
- Hardeman RR, Przedworski JM, Burke SE, Burgess DJ, Phelan SM, Dovidio JF, et al. Mental well-being in first year medical students: A comparison by race and gender: A report from the medical student CHANGE study. J Racial Ethn Health Disparities. 2015 Sep;2(3):403–13.
- Hendricks ML, Testa RJ. A conceptual framework for clinical work with transgender and gender nonconforming clients: An adaptation of the Minority Stress Model. Prof Psychol Res Pract. 2012 Oct;43(5):460–7.
- Breastfeeding and lactation for medical trainees. American Academy of Family Physicians (AAFP). 2019. Available at: https://www.aafp.org/about/policies/all/breastfeeding-lactation-medical-trainees.html#:~:text=As%20consistent%20with%20hospital%20policy,bodily%20fluid%20requiring%20universal%20precautions.
- Parental leave during residency training. American Academy of Family Physicians (AAFP). 2022, Sept. Available at: https://www.aafp.org/about/policies/all/parental-leave.html
- Paid parental leave: statement of policy. The American College of Obstetricians and Gynecologists (ACOG). 2023, Nov. Available at: https://www.acog.org/clinical-information/policy-and-position-statements/statements-of-policy/2020/paid-parental-leave
- Paid family leave and FMLA. American Academy of Pediatrics (AAP). 2023, Oct 2. Available at: https://www.aap.org/en/career-resources/conducting-your-job-search/paid-family-leave-and-fmla/#:~:text=Parental%20leave%20is%20essential,who%20takes%20maternity%2Fpaternity%20leave.
- Kesselheim AS, Austad KE. Residents: Workers or students in the eyes of the law? New England Journal of Medicine. 2011 Feb 24;364(8):697–9.
- Dyrbye LN, West CP, Satele D, Boone S, Tan L, Sloan J, et al. Burnout among U.S. medical students, residents, and early career physicians relative to the general U.S. population. Acad Med. 2014 Mar;89(3):443–51.
- Worly B, Verbeck N, Walker C, Clinchot DM. Burnout, perceived stress, and empathic concern: Differences in female and male Millennial medical students. Psychol Health Med. 2019 Apr 21;24(4):429–38.
Open Access
Peer-Reviewed
Creative Commons
Submitted: 24 June 2024
Accepted: 12 June 2025
Published: 18 July 2025
Conflicts of Interest: The authors declare no conflicts of interest.